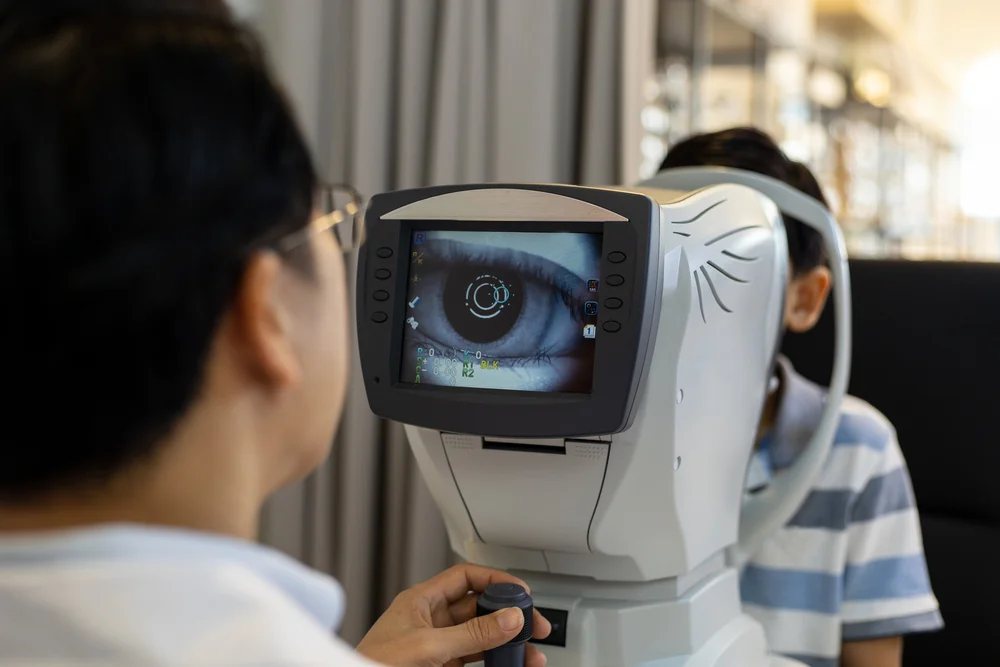
Ophthalmologist skills play a major role in protecting and restoring sight. An ophthalmologist is a medical doctor who treats eye diseases, performs surgery, and manages long-term vision care. In the United States, millions of people live with eye conditions like glaucoma, cataracts, and diabetic eye disease. The right skills can mean the difference between early treatment and permanent vision loss.
According to the Centers for Disease Control and Prevention, about 12 million people aged 40 and older have vision impairment. As the population ages, that number is expected to rise. This makes ophthalmologist competencies more important than ever. Patients want eye doctors who are skilled, careful, and easy to talk to.
In this article, you will learn about the essential skills for ophthalmologists, from eye examination techniques to surgical skills in ophthalmology. You will also see how patient communication and vision care management shape better outcomes.

What Are the Most Important Ophthalmologist Skills?
When people think about ophthalmologists, surgery is often the first thing that comes to mind. While surgical expertise is essential, the role of an ophthalmologist is far more comprehensive. It combines advanced medical knowledge, technical precision, and compassionate patient care. Strong ophthalmology expertise includes:
1. Deep Clinical Knowledge
An ophthalmologist must have a thorough understanding of eye anatomy, physiology, and disease. This includes recognizing and managing conditions such as cataracts, glaucoma, macular degeneration, diabetic retinopathy, and other complex ocular disorders.
2. Accurate Diagnostic Skills
Precise diagnosis is the foundation of effective treatment. Ophthalmologists must interpret imaging tests, visual field exams, and clinical findings to identify problems early and accurately.
3. Surgical Precision
Many ophthalmologists perform delicate microsurgeries. Excellent hand–eye coordination, steady hands, and attention to detail are critical to achieving safe and successful surgical outcomes.
4. Clear Patient Communication
Explaining diagnoses, treatment options, risks, and long-term care plans in understandable terms is essential. Patients need clarity and reassurance when facing vision-related concerns.
5. Careful Treatment Planning
Every patient’s condition is unique. Ophthalmologists must evaluate multiple factors—age, overall health, lifestyle, and disease progression—to create personalized treatment strategies.
6. Long-Term Vision Care Management
Many eye conditions require ongoing monitoring and management. Strong follow-up systems and preventive care strategies help preserve vision and maintain quality of life.
In summary, being an ophthalmologist requires far more than surgical skill. It demands medical expertise, analytical thinking, precision, communication, and a long-term commitment to protecting patients’ vision.
Why Are Clinical Skills in Ophthalmology So Important?
Clinical skills in ophthalmology are the foundation of safe, effective, and vision-preserving care. Before any laser procedure, injection, or surgery is performed, an ophthalmologist must first correctly identify the problem. Accurate clinical evaluation guides every treatment decision that follows.
Many serious eye diseases—such as age-related macular degeneration and diabetic retinopathy—develop gradually and may show few or no early symptoms. According to the National Eye Institute, research shows that while early preventive treatment for diabetic retinopathy can slow disease progression, careful monitoring and timely treatment when complications arise are key to preventing vision loss.
This highlights a crucial point: strong clinical judgment and regular assessment matter just as much as advanced technology.
In fact, diabetic eye disease often presents without noticeable symptoms in its early stages, making comprehensive eye exams essential for early detection. Without solid clinical evaluation, these silent conditions can progress to irreversible damage.
Core Clinical Skills Every Ophthalmologist Must Master
To detect and manage eye disease effectively, an ophthalmologist must:
- Take a detailed patient history: Understanding symptom patterns, family history, medications, and lifestyle factors provides vital diagnostic clues.
- Review systemic medical conditions: Diseases such as diabetes and hypertension significantly affect eye health. Diabetic retinopathy, for example, results from damage to retinal blood vessels caused by prolonged high blood sugar.
- Perform a comprehensive physical and ocular examination: Dilated eye exams can reveal early retinal bleeding, macular edema, or abnormal blood vessels before symptoms appear.
- Interpret diagnostic testing accurately: Imaging tools such as optical coherence tomography (OCT) and fluorescein angiography support diagnosis—but they only become useful when guided by proper clinical reasoning.
Why Clinical Judgment Matters More Than Technology Alone
Modern ophthalmology benefits from innovations such as AI-assisted screening tools that can detect diabetic retinopathy with high accuracy. However, even the most advanced systems depend on skilled clinicians to interpret findings, confirm diagnoses, and determine appropriate next steps. Technology enhances care—but it does not replace clinical expertise.
How Do Ophthalmic Diagnostic Skills Support Accurate Eye Disease Diagnosis?
Ophthalmic diagnostic skills go far beyond reading a vision chart. They involve a combination of technical expertise, clinical observation, and critical thinking. Accurate eye disease diagnosis depends on a physician’s ability to detect subtle changes—often before symptoms appear.
Strong diagnostic ability allows ophthalmologists to identify disease early, monitor progression, and choose the most effective treatment plan.
Why Attention to Detail Is Critical
Many serious eye diseases develop silently. Glaucoma, for example, often has no early symptoms. Vision loss may occur gradually and go unnoticed until significant damage has already been experienced. The ophthalmologist must recognize small structural changes in the optic nerve or subtle visual field defects long before the patient reports a problem.
The Role of Artificial Intelligence in Eye Diagnosis
In recent years, artificial intelligence (AI) tools have been introduced in U.S. clinics to assist in detecting conditions such as diabetic retinopathy. These systems can analyze retinal images and flag abnormalities. While promising, AI does not replace physician expertise.
Technology can support screening and efficiency—but final diagnosis, treatment decisions, and patient counseling still depend on human clinical judgment.
Why Hands-On Diagnostic Experience Matters
From reviewing physician resumes, one pattern is clear: candidates who highlight hands-on diagnostic experience stand out. Employers look for concrete examples of clinical exposure—interpreting imaging, performing tonometry, managing glaucoma patients, or diagnosing retinal disease.
Listing equipment proficiency is helpful. Demonstrating real-world application is even more powerful. To know more, check the expert tips for a successful medical resume.
Showing Strong Clinical Foundations through Medical Resumes
For medical professionals exploring or advancing in ophthalmology, developing strong clinical skills is non-negotiable. Mastery in history-taking, examination techniques, disease recognition, and long-term patient monitoring forms the backbone of exceptional eye care.If you are pursuing a healthcare career or looking to strengthen your professional profile, you can explore career guidance and industry insights at ResuMeds’ Medical Career Hub, which offers expert advice for healthcare professionals across specialties. Alternatively, you may want to seek help from professional resume writers specializing in healthcare resumes.
